Bar code system aids medical precision
Last year, Lawrence Memorial Hospital’s medication error rate was less than one mistake out of every 10,000 dosages that reached a patient.
That’s not a lot, but Pat Parker says it’s still too many.
“One is too many,” said Parker, director of pharmacy and IV therapy at LMH.
Last May, LMH installed a state-of-the-art bar-code system for making sure the right patients gets the right dosages of the right medications at the right time.
Though about 10 percent of the nation’s hospitals have started using bar codes to keep track of patients and their drugs, LMH’s system is one of only a handful that gives doctors and nurses access to real-time information on when medications are given.
“We’re very much on the cutting edge,” Parker said. “We’ve taken – and we continue to take – a lot of steps to make medication usage safer for our patients. This is a very big step.”
Last year, a national Institute of Medicine study found that 7,000 people die each year because of hospital-based drug errors.
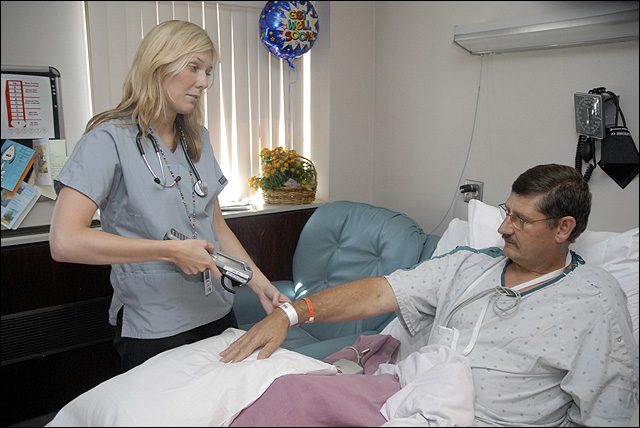
Jessica Wright, left, a registered nurse, checks Mark Warren's bar code on his bracelet at Lawrence Memorial Hospital. The hospital switched to a bar code system to keep track of patients and their medications last May. Wright checked Warren's bar code on Wednesday.
“In my 20-plus years here at LMH, that’s not happened,” Parker said. “But that doesn’t mean it couldn’t happen, and that’s what is driving up to this process.”
Here’s how the new LMH system works:
¢ When a patient is admitted, their medical information is entered into a computer system, which, in turn, generates a bar code. The bar code – which looks like a miniature crossword puzzle – is added to the patient’s wristband.
¢ Every medication dispensed at LMH is now bar-coded.
¢ Before a patient is given a pill, a shot or an IV, the bar codes are scanned using hand-held scanners. The patient’s wristband, too, is scanned. If there’s an error, the scanner alerts the nurse before the medication reaches the patient.
¢ The system also warns the hospital’s pharmacy when a patient’s doctors prescribe conflicting medications.
¢ As soon as a medication is given, the information is readily accessible to the patient’s doctor and to the hospital’s medical and pharmacy staffs.
“Under the old pen-and-paper way of doing things, only two people knew when a medication was given – the patient and the nurse. If someone else needed to find out, they’d have to track down the patient’s chart,” Parker said. “Now, it’s in real-time. A doctor can be in his or her office and see which medications have been given and when.”
Many hospitals use bar codes, but their efforts often are hampered by scanners not working on curved surfaces, Parker said. And not all drug companies, he said, are bar-coding their products.
At LMH, the pharmacy staff puts a flat-surface bar code on hundreds of medications before they reach the patients. Each is triple-checked before it leaves the pharmacy.
To get around the curved-surface problem, the hospital uses a bar code that fits in a 1/8-inch square.
“The system makes it very hard to make a medications error,” said Dana Hale, vice president of nursing at LMH. “If I try to give the patient in Bed 1’s pill to the patient in Bed 2, the system tells me not to.”
Currently, LMH has 60 hand-held scanners. Each floor has several computers that give nurses quick and easy access to the data.
“It’s great,” said Jessica Wright, a second-floor medical unit nurse. “At first, the learning curve was pretty steep, but we’re all acclimated now. This isn’t something we do once every three or four weeks – we’re doing it many, many times a day. You learn pretty quick.”
Plans call for adding patients’ vital signs – temperature, pulse, respiration rate and blood pressure – to the system by year’s end.






